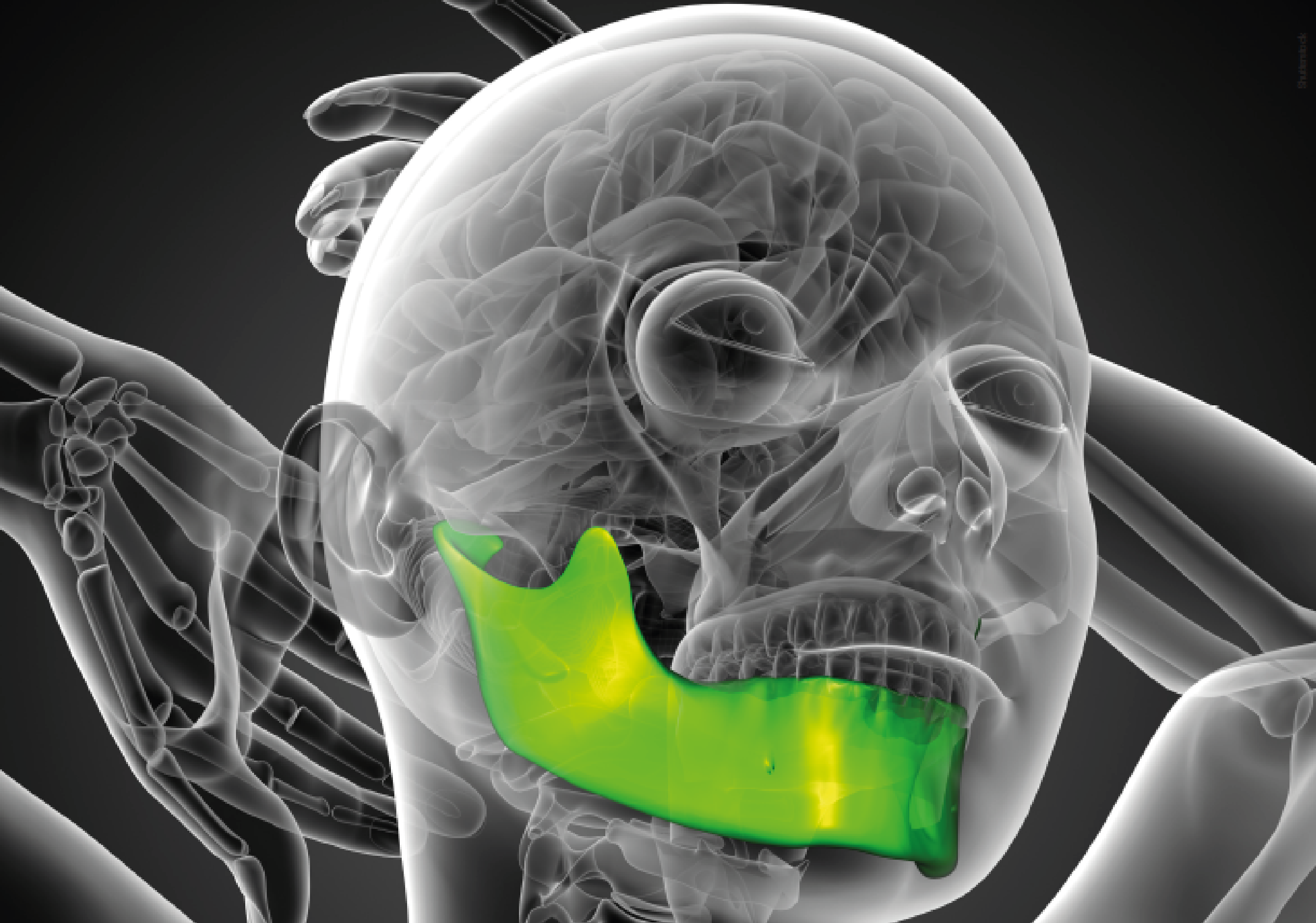
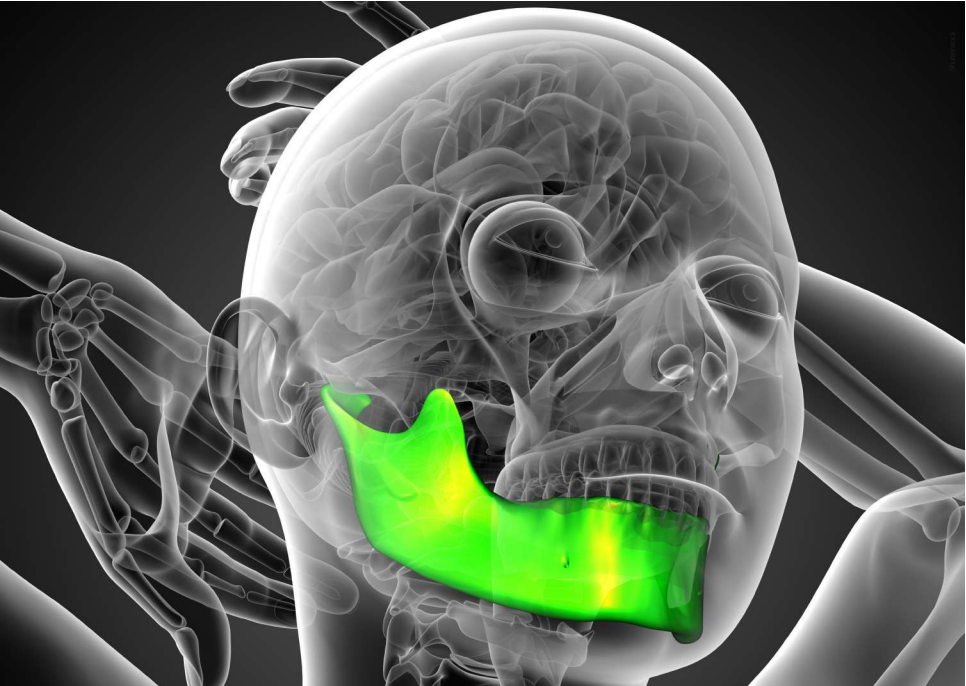
3D Imaging Exams and Advances in Joint Prosthesis Studies are the Key Differentiators in TMJ Disorder Treatments.
Among the recognized causes of orofacial pain in dentistry, temporomandibular joint disorder (TMJ) is one of the most prevalent issues affecting the global population. According to the 1st Consensus on Temporomandibular Dysfunction and Orofacial Pain, approved in 2010, it is estimated that around 37% of individuals in Brazil present at least one symptom of this problem.
There have been significant advancements in the study of TMJ disorders. Experts have identified new methods for accurate diagnosis and more effective treatments, ranging from initial patient assessments to complex cases, which ultimately enhance the quality of life for patients. It is essential that the entire dental community, not just specialists, remains attentive to this issue.
Ideally, every dentist, regardless of their specialty, should be able to identify TMJ disorders. To achieve this, understanding the signs and symptoms (see box) is crucial. Typically, patients with this disorder are recommended to seek treatment from a specialist to ensure proper care.
Diagnosis
Currently, dental professionals have advanced systems at their disposal that allow for comprehensive and detailed analysis of the temporomandibular joints (TMJs) through 3D imaging generated by tomography scans. The use of specific software enables various cross-sections of the captured image, as well as the ability to view it from different angles. “The advent of 3D imaging has provided us with an in-depth view of the intra-articular structures, which allows for a better understanding of TMJ issues and consequently provides greater possibilities for stabilizing the dysfunctional process,” says Dr. Luiz Fernando Lobo, a specialist in Oral and Maxillofacial Surgery and Head of the Oral and Maxillofacial Surgery Service and Residency Program at Hospital Santa Paula in São Paulo.
Dental treatments can be compromised if TMJ disorders (TMJD) are not diagnosed.
Complementary exams can be used in conjunction with tomography to provide a more accurate diagnosis and faster treatment results. Electromyography can be utilized for muscle analysis, which involves identifying how facial muscles are functioning and detecting inflammation through strategically placed electrodes.
Other systems, such as Joint Movement Analysis (JMA) and Joint Vibration Analysis (JVA), also provide computerized evaluations of the jaw by analyzing movement and vibration. These exams can be outsourced, but specialized clinics are already incorporating these procedures into TMJD treatment.
Clinical Treatments
The priority in treating TMJ disorders (TMJD) is to alleviate the patient’s pain. Even if surgical intervention is needed later on, clinical treatment is the initial step. The objectives are to eliminate muscular and joint inflammation and improve the range of jaw movements. In some cases, it’s even possible to reposition the jaw.
This procedure is based on the use of an interocclusal splint. According to Dr. Guiovaldo Paiva, a specialist in Orofacial Pain and Temporomandibular Dysfunction and co-founder of the ATM Diagnostic and Treatment Center, the thickness and appropriate type of splint are determined by the professional based on the established diagnosis. “To enhance the effectiveness of this first phase, we also recommend ATM physiotherapy, which involves applications of low-intensity laser, ultrasound, and muscle exercises,” he explains.
After restoring the functional system of the joint, the patient will move on to the second phase. In most cases, this process will be guided by orthodontics, and if necessary, implantology can also be included. However, it’s crucial to ensure that the first phase is successfully completed. “We cannot ignore TMJs before initiating any dental treatment, as any treatment done by other specialties could be compromised if there’s dysfunction,” Dr. Guiovaldo Paiva explains.
Today, in addition to using the interocclusal splint, some professionals use botulinum toxin type A as a minimally invasive therapy, applied to specific muscle points. According to Dr. Tarley Pessoa de Barros, PhD in Dentistry from the University of São Paulo and specialist in Oral and Maxillofacial Surgery, the toxin acts at the neuromuscular junction, preventing the release of acetylcholine and thus muscle contraction.
The specialist explains that he considers this one of the most effective alternatives because the substance is a potent muscle relaxant. He notes that the inconvenience is the need for reapplication. “The therapy has quick action and minimal or almost nonexistent side effects, as long as the patient is not allergic to the components of the formula, is not pregnant or lactating, and does not have neuromuscular disease,” says Dr. Barros.
A study conducted by Allergan, the manufacturer of Botox® in Brazil, showed that the toxin, applied to patients diagnosed with bruxism, has led to a 50% reduction in pain episodes and has also improved sleep quality.
Although the therapeutic use of toxin in dental procedures was approved by the Brazilian Federal Council of Dentistry in 2014, opinions on the topic still vary, with some advocating for more evidence-based studies.
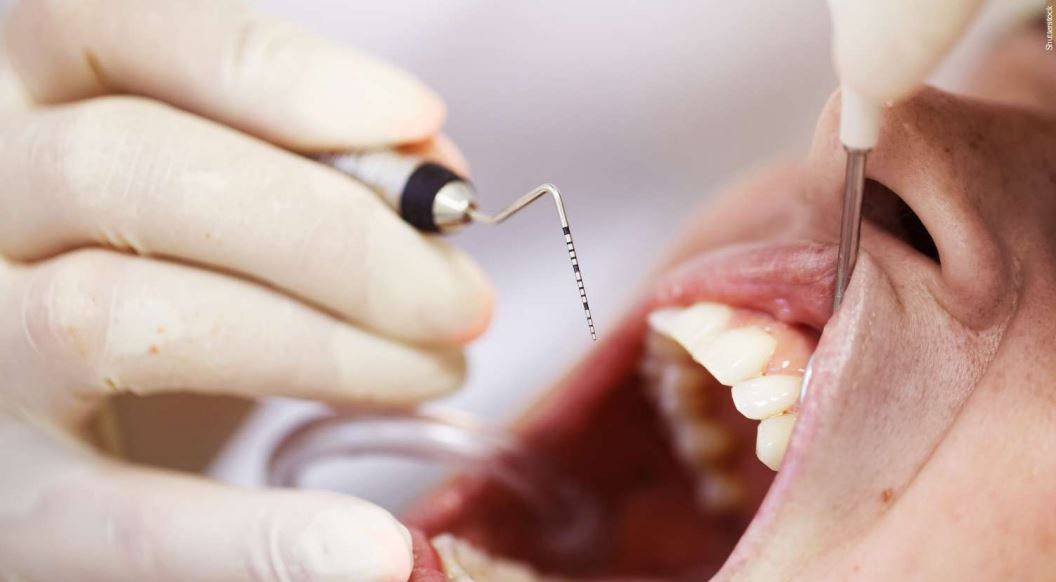
Surgical Intervention
For more severe dysfunctions, the use of joint prostheses has gained prominence. Currently, Brazil is among the most advanced countries in this field. Prostheses allow for the repair of TMJs while preserving joint movement. “This option is indicated in severe cases of osteoarthritis and allows for greater control of the quality of movement, which was not possible in other procedures,” explains Dr. Luiz Fernando Lobo. However, the specialist emphasizes that the entire TMJD treatment procedure must undergo prior clinical processes.
“You cannot predefine the cases that should be referred for surgery, but there are proposed classifications that aid in daily clinical practice,” says Dr. Lobo. These may include cases of articular disc displacement with reduction or with persistent reduction accompanied by clicking and noise, disc displacement without reduction, and severe osteoarthritis with limited mobility.
Lack of Diagnosis – In addition to compromising other dental treatments, untreated TMJD can even trigger depression. “Many patients experience manifestations of irritability, hyperactivity, or repetitive movements, which can be classified as anxiety,” explains Dr. Luiz Fernando Lobo.
In addition to psychologists and psychiatrists, other specialists such as physiotherapists can be included in the TMJD treatment when muscle stretching is required, and speech therapists can help improve joint movement.
“We now recognize the importance of involving other areas of health in this process, as well as other dental specialties such as orthodontics and prosthodontics,” concludes Dr. Tarley Pessoa de Barros, PhD in Dentistry from the University of São Paulo and specialist in Oral and Maxillofacial Surgery.
On the Path to Diagnosis
The origin of TMJD is multifactorial. According to the 1st Consensus on Temporomandibular Dysfunction and Orofacial Pain, factors can be of traumatic origin, psychosocial (anxiety and depression), and physiopathological (systemic diseases, altered intra-articular pressure, and genetics). What will define the diagnosis are the symptoms presented by the patient and the signs identified in clinical examinations.
TMJD Symptoms – Patients
- Pain in the face, TMJs, and chewing muscles;
- Headaches and earaches, and;
- Otolaryngologic manifestations – tinnitus, vertigo, and sounds perceived in a muffled manner.
TMJD Signs – Clinical Examination
- Muscular and TMJ tenderness,
- Limitation or coordination issues in jaw movements,
- Joint noises,
- Incorrect teeth positioning
According to Dr. Guiovaldo Paiva, a specialist in Orofacial Pain and Temporomandibular Dysfunction and co-founder of the ATM Diagnosis and Treatment Center, in addition to checking for the most common symptoms, the dentist should also inquire about recent or past accidents, previous dental treatments – especially orthodontics – and also inquire about the patient’s sleep. ‘It is very important to know if the patient sleeps well, as we know that obstructive sleep apnea may be related to TMD, and imaging tests will allow us to also evaluate the upper airway, where the oropharynx is located, which could potentially block the airway,’ he says.
In order for the information to be analyzed more accurately and result in a more comprehensive diagnosis, it is crucial for the patient to be referred for specialized care. ‘It is very rare for people to seek a specialist when they notice the signs and symptoms, so dentists need to conduct a more in-depth examination, identify the problem, and know who to refer them to,’ says Dr. Paiva.
Source: Journal of ABO 2015 (Edition 154 | August/September/October 2015)