INTRODUCTION
Dental caries, defined as localized destruction caused by bacterial action, still affects a significant portion of the population, especially children and young adults.1,2 Being considered an infectious disease with a multifactorial nature, strongly influenced by fermentable carbohydrates (e.g. sucrose, starch) in the diet, its control to prevent damage to dental structures can be challenging in certain situations.1-7 The occlusal surface represents a highly susceptible region for lesion initiation, where its grooves, pits, and fissures create an environment conducive to its development. This clinical condition is exacerbated by the difficulty of maintaining hygiene in this area (Fig. 1).5 In line with these findings, dental caries lesions can begin in pits and fissures shortly after tooth eruption, and if not prevented or treated, can lead to tooth loss over time.1,2
One form of prevention involves the mechanical sealing of structural enamel defects through the proper application of a resin-based, glass ionomer, or resin-modified glass ionomer pit and fissure sealant. According to various longitudinal clinical studies, these sealants have proven to be excellent, safe, durable, and effective preventive alternatives for inhibiting the onset and progression of the disease, thereby significantly controlling cariogenic activity in this region.1-4,6,7,8,9 Therefore, the aim of this work is to present a scientifically supported clinical protocol for the application technique of a resin-based pit and fissure sealant.

CLINICAL PROTOCOL
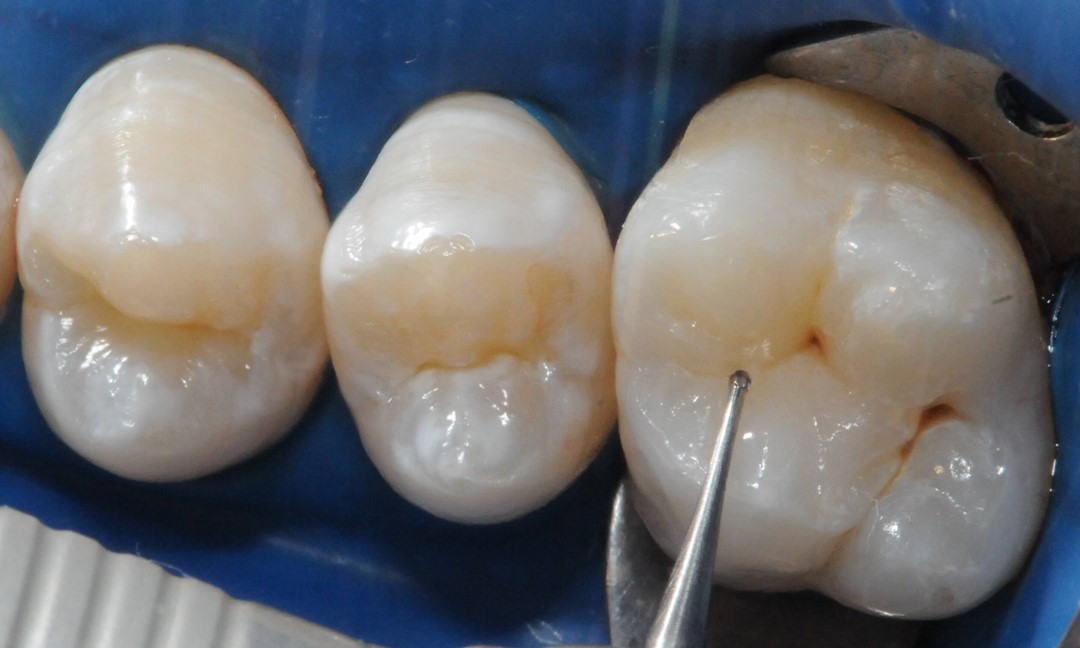
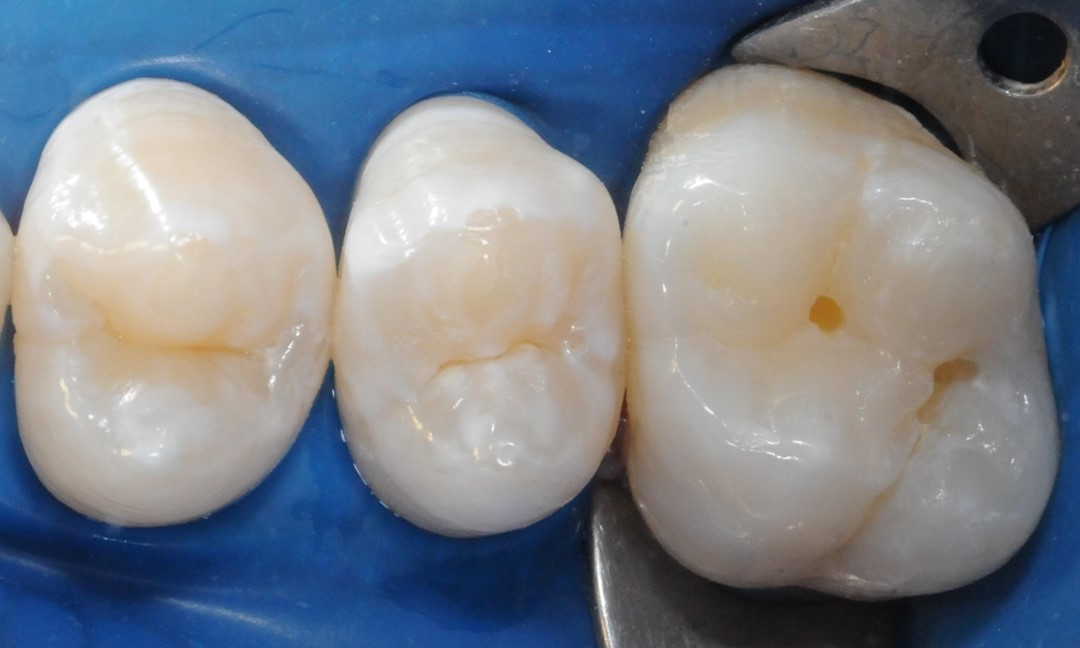
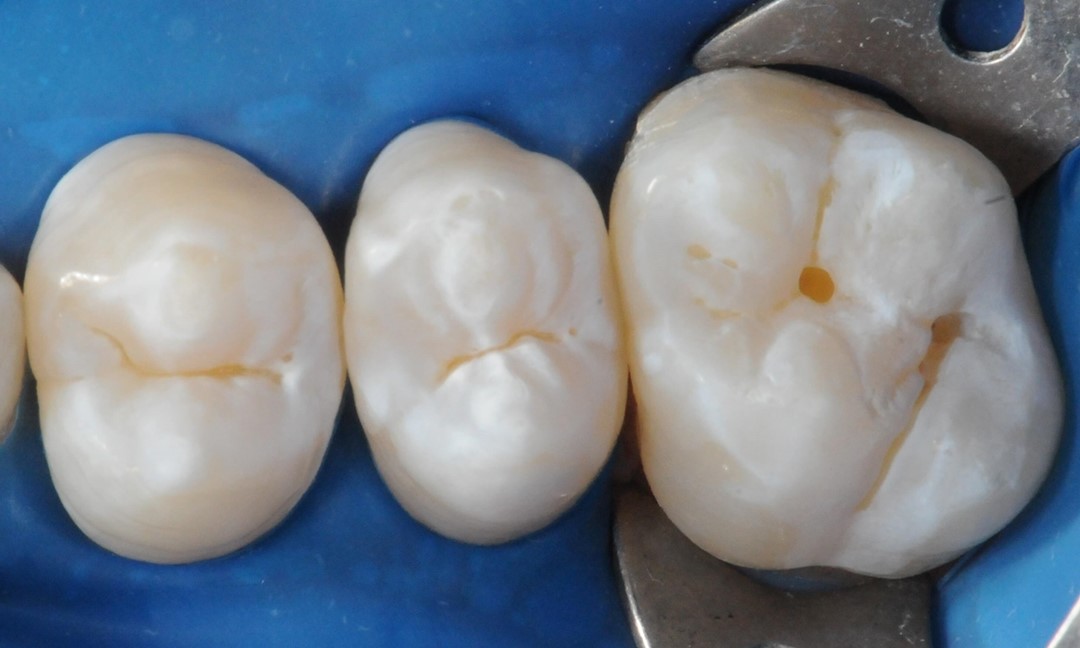
The sealing technique begins with absolute isolation of the operative field (Fig. 2), when possible; followed by dental prophylaxis using pumice and water. We must emphasize the need for minimally invasive technique application for grooves and fissures with localized chromatic changes, by using a carbide ¼ spherical bur (KG Sorensen Indústria e Comércio Ltda, Barueri, São Paulo, Brazil) only on the grooves and fissures with chromatic changes prior to occlusal sealing (Fig. 3 and 4).

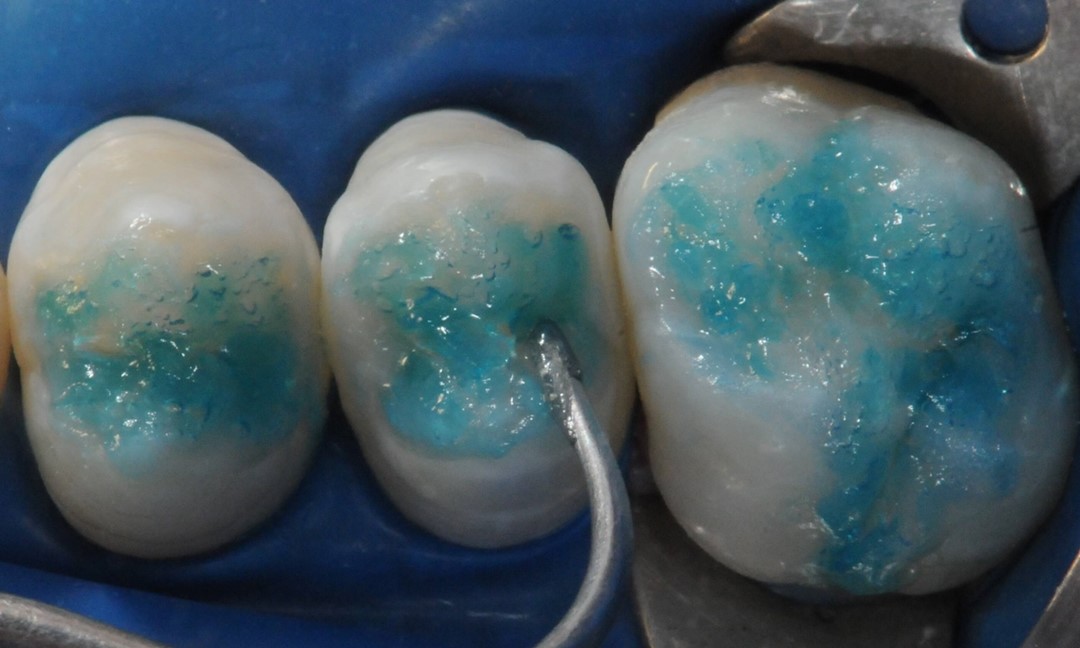
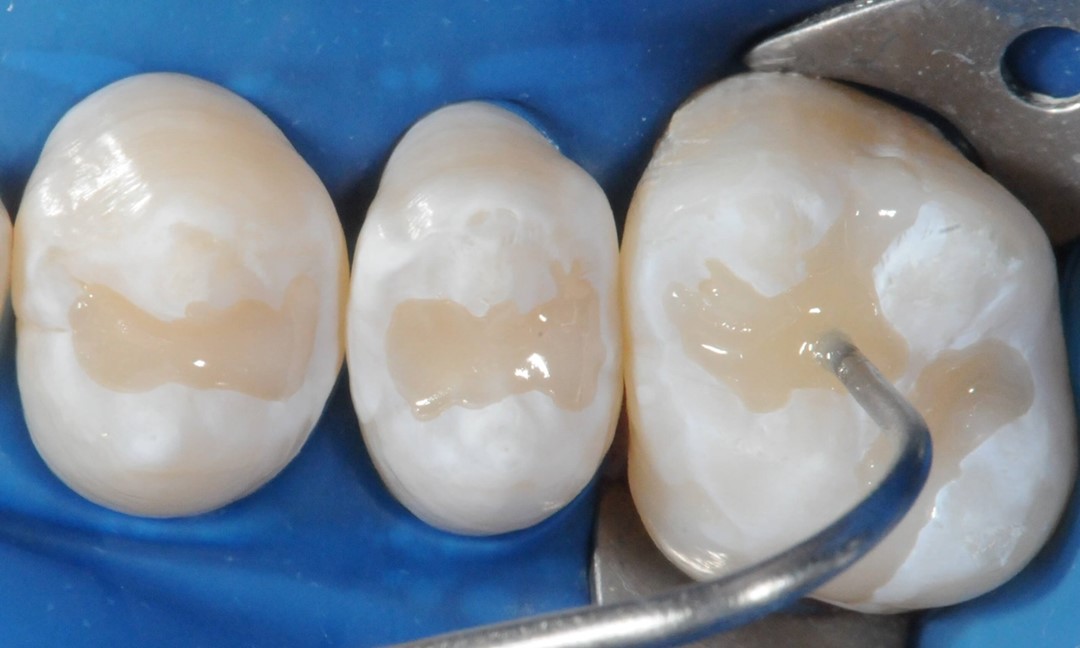
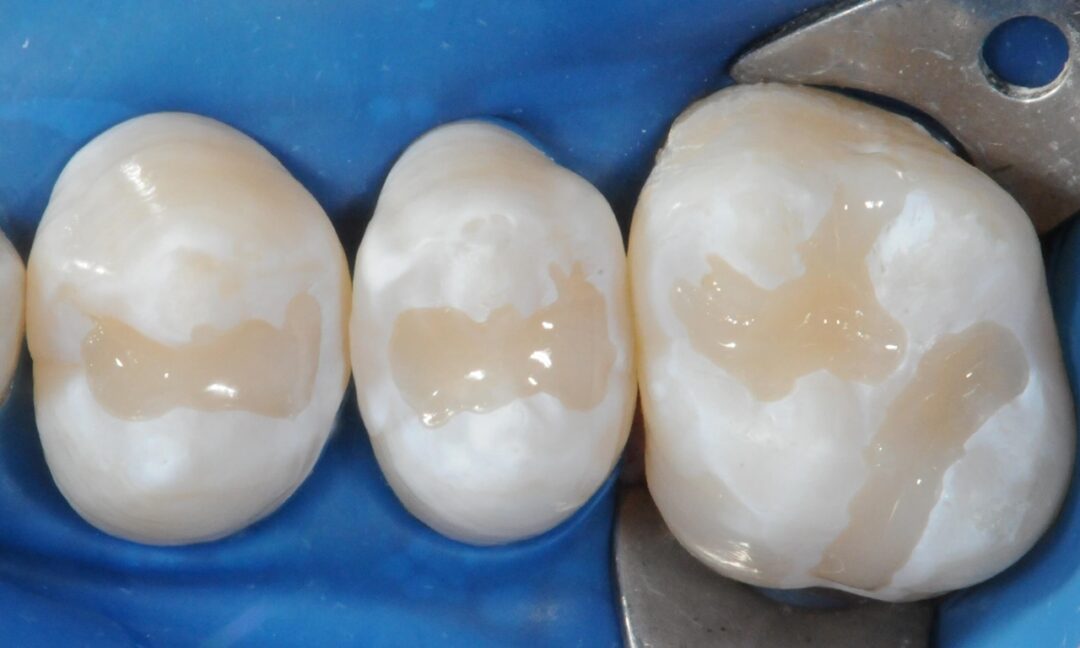
Next, after prophylaxis (Fig. 5), enamel conditioning is performed on the entire occlusal surface using 37% phosphoric acid (Condac 37, FGM) in gel form, with vibration, employing an explorer probe for a duration of 30 seconds (Fig. 6). After thorough rinsing with water and air drying (Fig. 7), the sealing material (Prevent, FGM) should be applied in all grooves and pits using an explorer probe with vibration assistance (Fig. 8).
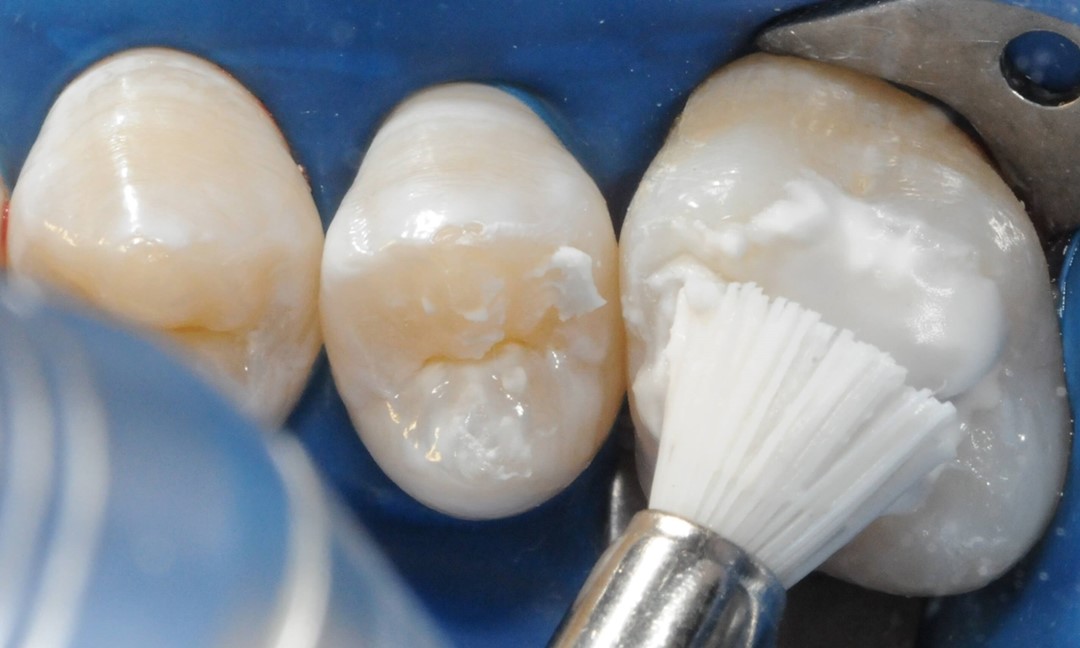
Photopolymerization will be carried out for 20 seconds, using a halogen or LED light source with appropriate light intensity, at a power of over 400 mW/cm² (Fig. 9). When necessary, occlusal adjustment should be performed in maximum habitual intercuspation, with the patient seated and the occlusal plane parallel to the ground, using a carbon strip. Premature contacts, if present, should be removed with a diamond bur numbered 1014 (K.G. Sorensen), mounted on a high-speed handpiece, with water and air cooling, followed by the action of an abrasive rubber point.
DISCUSSION
According to clinical studies by Sundfeld et al. in 1990, 1992, 1993, 2001, 2004, 2006, 2007, and 2010, in order to achieve proven clinical success in sealing grooves and fissures with a sealing material, whether resin-based or resin-modified glass ionomer, a thorough clinical examination of the occlusal surface and interproximal radiographs should be performed initially. Teeth considered suitable for fissure sealing should have clinically and radiographically intact proximal surfaces, accompanied by clinically and radiographically intact grooves and fissures, meaning clear grooves and fissures without chromatic changes. However, those presenting small localized chromatic changes,10 as in the present clinical protocol report, suggestive or not of incipient carious lesions, could receive sealant application only after the removal of these changes, using a carbide ½ or ¼ spherical bur (K.G. SORENSEN) mounted on a high-speed handpiece. It is worth noting that teeth exhibiting extensive carious lesions that affect the entire occlusal groove and/or dentin tissue and involve all pits and fissures are not suitable for the pit and fissure sealant technique.
Kramer et al. in 1991 and 1997 consider newly erupted teeth as ideal candidates for pit and fissure sealant application. Moreover, the concept that teeth that have not developed carious lesions within 2 years after eruption are not suitable for sealing is considered debatable. This perspective only considers post-eruptive maturation; however, an individual is not exempt from developing fissure and pit caries during the subsequent years, considering factors like oral hygiene, occlusal anatomy, diet, and other secondary and modifying factors that influence disease development. It’s important to emphasize that these factors can reverse a stabilized state of oral health, potentially transitioning a low-risk patient from caries-free to clinically active caries.13
It’s worth noting that the incorrect application of the principles underlying the sealing technique has been identified as the main and decisive factor in the failure of sealants. Therefore, if you choose to perform it, do it correctly; otherwise, refrain from doing so!1-4, 6-9
In 2001, Sundfeld highlighted that the excellent clinical performance presented by the occlusal sealants evaluated in his 11-year longitudinal clinical study is primarily grounded in the extremely precise technique to which they were subjected. He emphasized with great vigor that the material was applied to conditioned enamel that was thoroughly dry and uncontaminated. This fact certainly contributed to the substantial retention of the sealing materials used, as enamel conditioning was performed on the entire occlusal surface, preventing the application of the sealant to unconditioned enamel. This, undoubtedly, would lead to marginal infiltration around the sealant. He also noted the absence of total loss of the sealing material and of carious lesions around the sealants in this longitudinal clinical study, regardless of the type of sealing material used, whether it was resin-based alone or with fluoride in its composition.
However, it is advisable to conduct periodic interproximal radiographic examinations, as well as to emphasize oral hygiene control. It’s important to provide guidance on intelligent consumption of sucrose and fermentable carbohydrates to prevent lesion development on proximal surfaces. This clearly demonstrates that dental caries is a multifactorial condition, where each factor has its specific role, requiring their interaction for the carious process to initiate.1,2
In this context, occlusal sealing indeed represents a significantly substantial advancement in eradicating dental caries and enamel structural defects. It offers numerous benefits, such as painless application, good clinical acceptance, and being considered a conservative adhesive procedure.
CONCLUSION
In conclusion, the application of pit and fissure sealants through an appropriate technique undeniably constitutes an effective and safe resource in the prevention of pit and fissure caries lesions.
GALLERY
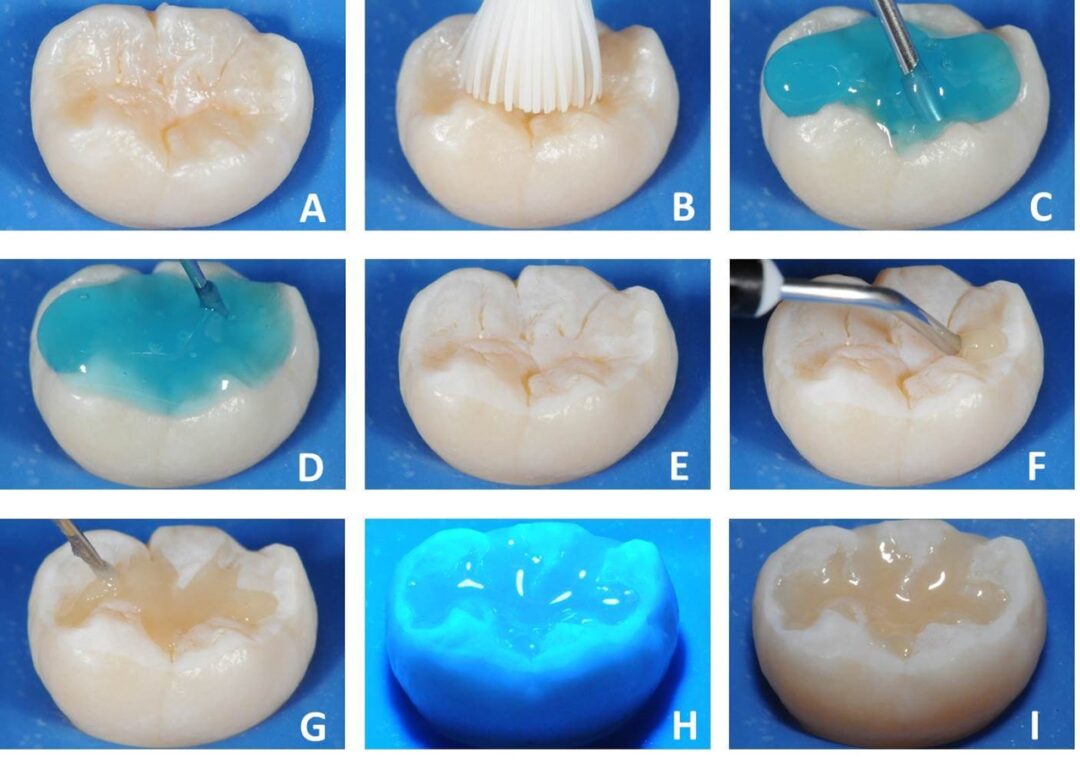
Laboratory Sequence for Observation of Resin Tags Under Common Optical Microscopy with Polarized Light. A – Grooves, pits, and fissures of an extracted molar; B – Prophylaxis with pumice and water; C – Conditioning with 37% phosphoric acid (Condac 37, FGM); D – Complete conditioning for 30 seconds; E – Opaque whitish appearance of enamel after conditioning; F – Application of sealant (Prevent, FGM); G – Applying over the entire area of pits and fissures; H – Photopolymerization for 20 seconds; I – After fissure sealing, the tooth was sectioned using a high-precision cutter, and the slices were polished to observe the adaptation of the sealant and resin tags under common optical microscopy with polarized light.
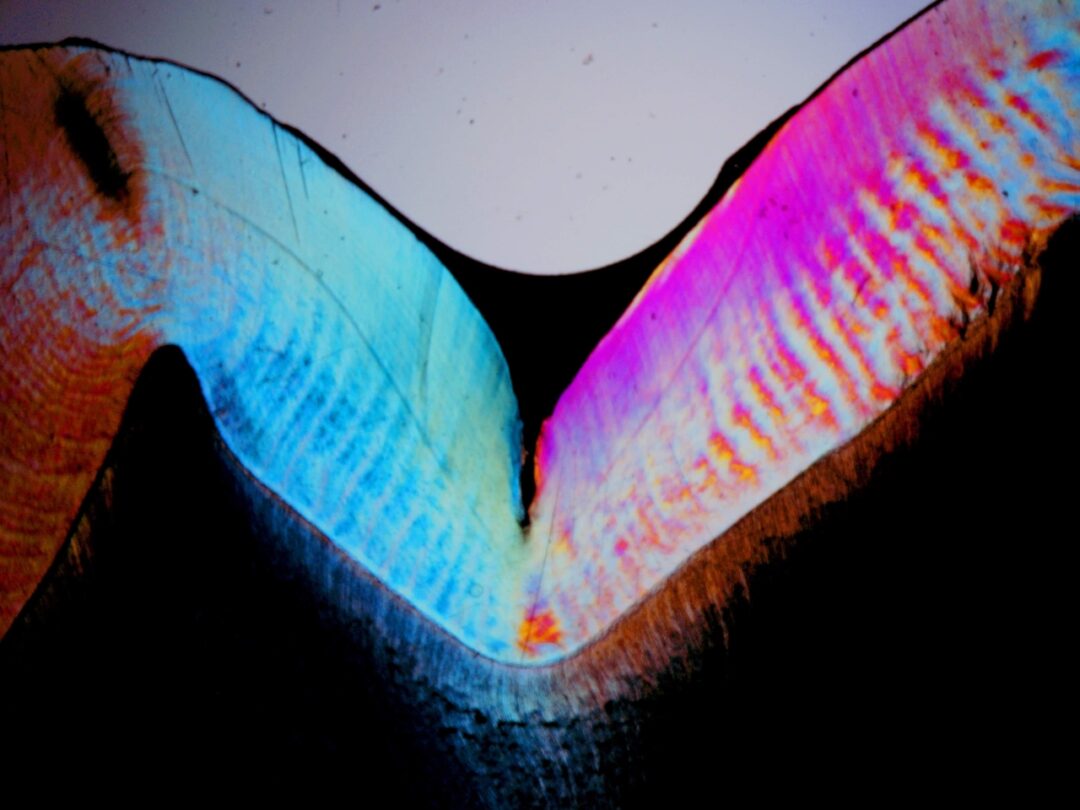
Sectioning by wear of the posterior tooth sealed with Prevent pit and fissure sealant (FGM).
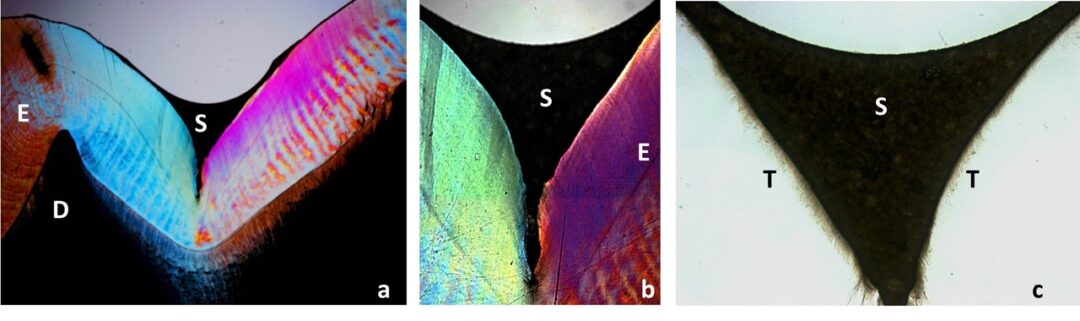
Sequence observing the adaptation of Prevent sealant (FGM) in the groove and the resinous extensions (tags) responsible for the mechanical bonding of the pit and fissure sealant to the enamel. (E) enamel (D) dentin (S) Prevent pit and fissure sealant (FGM) and (T) tags. Photos (a) at 25x magnification, (b) at 50x magnification, and (c) after enamel decalcification at 100x magnification.

After observing the sealant adaptation, the tooth was decalcified to observe the resinous extensions formed by Prevent sealant (FGM) on the enamel. (T) – resinous extensions (tags) responsible for the mechanical bonding of the pit and fissure sealant to the enamel.
REFERENCES
- Sundfeld, R.H. Análise microscópica da penetração ―in vivo‖ de selantes de fóssulas e fissuras; efeitos de tratamentos superficiais e materiais. Araraquara, 1990. 1 46p. Tese (Doutorado) — Faculdade de Odontologia de Araçatuba, Universidade Estadual Paulista.
- Sundfeld, R.H. A eficiência da aplicação de selantes na prevenção das lesões de fóssulas e fissuras: análise clínico-fotográfica e clínico-computadorizada. Araçatuba, 2001. 277p. (Tese Livre Docência) — Faculdade de Odontologia de Araçatuba, Universidade Estadual Paulista.
- Sundfeld RH, Mauro SJ, Komatsu J, Rahal S. Retenção dos selantes: avaliação clínica fotográfica: 18 meses de análise. RGO, v.40, n.6, p.424-6, 1992.
- Sundfeld RH, Mauro SJ, Komatsu J, Rahal S. Análise clínica fotográfica da retenção de selantes de fóssulas e fissuras: 36 meses de análise. Âmbito Odontol, v.3, n.14, p.334-9, 1993.
- Serra MC, Pimenta LAF, Paulillo LAMS. Dentística e manutenção de saúde bucal. IN: KRIEGER, L. ABOPREV. Promoção de saúde bucal. 2.ed. São Paulo: Artes Médicas, 1999. 475p.
- Sundfeld RH, Mauro SJ, Briso ALF, Sundefeld MLMM. Clinical/photographic evaluation of a single application of two sealants after eleven years. Bull Tokyo Dent Coll, v.45, n.2, p. 67-75, 2004.
- Sundfeld RH, Croll TP, Mauro SJ, Briso ALF, de Alexandre RS, Sundefeld MLMM. Longitudinal photographic observation of the occurrence of bubbles in pit and fissure sealants. J Appl Oral Sci, v.14, n.1, p.27-32, 2006.
- Sundfeld RH, Mauro SJ, Dezan E Jr, Sundefeld MLMM. Measurement of sealant surface area by clinical/computerized analysis: 11-year results. Quintessence Int, v.38, n.7, p.384-392, 2007.
- Sundfeld RH, Briso ALF, Mauro SJ, de Alexandre RS, Sundfeld Neto D, Oliveira FG, Machado LS. Twenty Years Experience with Pit and Fissure Sealants. Int J Clin Dent, v.2, n.4, p1-12, 2010.
- Eklund SA, Ismail AI. Time of development of occlusal and proximal lesions: implications for fissure sealants. J Public Health Dent, v.46, n.2, p.114-21, 1986.
- Kramer PF, Fernandes Neto PG, Fernandes RM, Corrêa MSNP, Fazzi R. Selantes oclusais: revisão da literatura: os selantes oclusais, seus aspectos clínicos e a importância de um programa de prevenção. Rev Assoc Paul Cir Dent, v.45, n.3, p.473-7, 1991.
- Kramer PF, Feldens CA, Romano AR. Promoção de saúde bucal em odontopediatria: diagnóstico, prevenção e tratamento da cárie oclusal. 2.ed. São Paulo: ArtesMédicas, 1997. 144p
- Croll TP & Sundfeld RH. Resin-based composite reinforced sealant. J Dent ChiId, v.66, n.4, p.233-8, 1999.